OxyContin may seem like a lifesaver for those in need of long-term pain treatment. However, for many people struggling to quit this drug due to distressing OxyContin withdrawal symptoms, it is the exact opposite of that.
Unfortunately, thousands—if not millions—of Americans find it nearly impossible to stop taking OxyContin due to developing a dependence on it.
Even though anyone can become dependent on this drug, recovery is possible. Detoxing from OxyContin the right way can help minimize uncomfortable withdrawal symptoms and pave the way for long-term recovery.
What Is OxyContin?
OxyContin is an extended-release formulation of oxycodone, a potent semi-synthetic opioid used to relieve moderate or severe pain, such as after surgeries. Due to the high potential for abuse, dependence, and addiction, it is usually only prescribed when the pain is long-lasting and resistant to non-opioid painkillers, such as aspirin or ibuprofen.
Other brand names oxycodone is commonly marketed under include:
- Oxaydo®
- Roxicodone®
- Oxydose®
As an extended-release medication, OxyContin is sold in the form of tablets. Once taken, they gradually release the drug into the system over 12 hours.
Like all prescription opioids, OxyContin works by interacting with opioid receptors in the central nervous system (CNS). By attaching to these receptors, it inhibits the transmission of pain signals between the body and the brain, resulting in reduced sensation of pain. This way, OxyContin mimics endorphins—neurotransmitters known as the body’s natural pain relievers.
OxyContin also triggers dopamine release—you may feel very relaxed and even euphoric after taking it, which makes this drug highly addictive.
OxyContin Withdrawal Symptoms
OxyContin withdrawal symptoms appear when people quit or reduce their oxycodone intake after developing a dependence on it.
Taking OxyContin regularly desensitizes your body to this medication. Due to increased tolerance to the drug, you’ll eventually need to up your OxyContin intake to feel its effects.
Tolerance is a sign of physical dependence on the drug, meaning you can no longer function normally without it. If you suddenly cut back or stop taking OxyContin altogether, your body will enter a state of OxyContin withdrawal, characterized by physical and psychological withdrawal symptoms.
Some physical OxyContin withdrawal symptoms include:
- Decreased appetite
- Diarrhea
- Dilated pupils
- Watery eyes
- Excessive yawning
- Fever
- Goosebumps
- Headache
- Increased pain sensitivity
- Muscle aches
- Nausea and vomiting
- OxyContin cravings
- Rapid heart rate
- Runny nose
- Stomach ache
- Tremors
Meanwhile, the most common psychological OxyContin withdrawal symptoms are:
- Agitation
- Anxiety
- Depression
- Dysphoria
- Mood swings
- Sweating
- Trouble falling or staying asleep
Some oxycodone withdrawal symptoms can be potentially life-threatening. They can also be very hard to bear, which increases the risk of relapse and opioid overdose. For this reason, it’s in your best interest to detox from OxyContin under medical care.
OxyContin Withdrawal Timeline
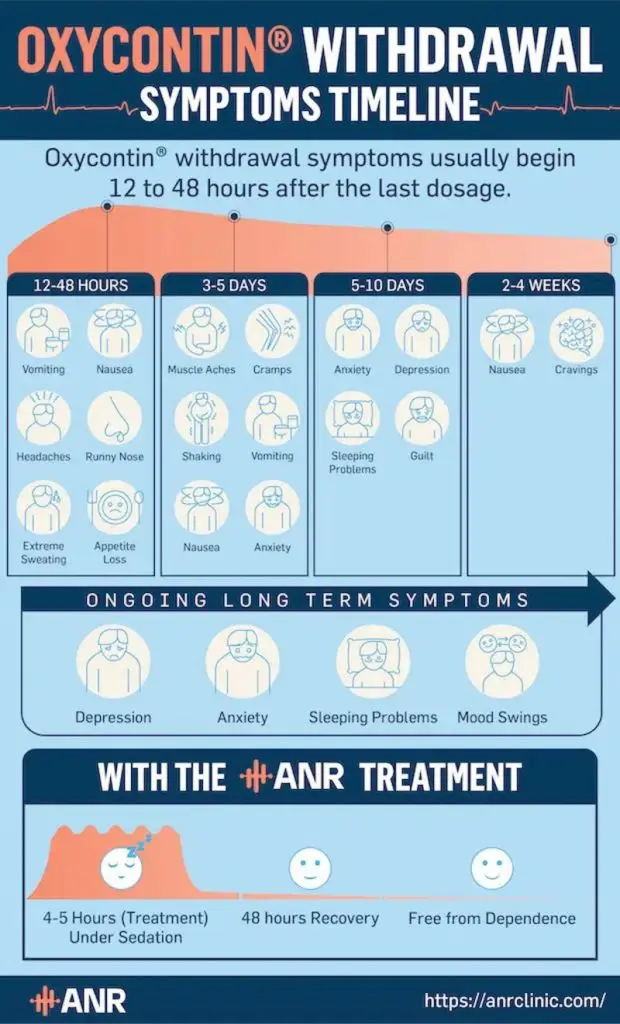
The OxyContin withdrawal timeline varies from person to person depending on the average dose, frequency of opioid use, metabolism, and other factors.
That said, since it’s a long-acting opioid, OxyContin withdrawal is typically longer than that of short-acting opioids, including immediate-release oxycodone.
Here’s what the typical OxyContin withdrawal timeline looks like:
Days 1–2
OxyContin withdrawal symptoms usually occur within the first 48 hours following the last dose, though in some cases, it may take up to four days for the first symptoms to appear.
The onset of OxyContin withdrawal is characterized by physical withdrawal symptoms, such as:
- Flu-like symptoms (fever, runny nose, headache, etc.)
- Nausea
- Vomiting
- Loss of appetite
Days 3–4
During this time, OxyContin withdrawal symptoms usually peak in intensity.
In addition to the withdrawal symptoms listed above, you may also experience tremors, muscle aches, OxyContin cravings, and other physical and psychological symptoms.
Days 5–14
Physical OxyContin withdrawal symptoms begin to slowly subside after reaching their peak. More often than not, they fade away within ten days, though some people may struggle with them for upwards of two weeks.
Although physical withdrawal symptoms usually get better during this time, most people will experience more intense psychological withdrawal symptoms after the first week of OxyContin withdrawal. Depression, anxiety, intense cravings, insomnia, and such can put you at a heightened risk of relapse during this time.
OxyContin Post-Acute Withdrawal Syndrome (PAWS)
OxyContin post-acute withdrawal syndrome (PAWS) is marked by withdrawal symptoms that persist for several weeks, months, and sometimes even years after quitting opioid use.
OxyContin is a long-acting opioid, so people who take it experience withdrawal symptoms for a longer time than those who take short-acting opioids. Nonetheless, acute OxyContin withdrawal symptoms typically subside within a couple of weeks.
However, some people experience withdrawal symptoms long after quitting OxyContin. Usually, PAWS symptoms are psychological, such as:
- Depression
- Irritability
- Anxiety
- OxyContin cravings
- Difficulty concentrating
- Impaired memory
- Sleep disturbances
- Mood swings
- Fatigue
- Poor impulse control
Coping with PAWS can be incredibly difficult and put you at risk of relapse. The good news is that receiving proper treatment for opioid addiction can help you prevent or overcome this syndrome.
How to Manage OxyContin Withdrawal Symptoms
If your withdrawal symptoms are relatively mild, you may be able to manage them with home remedies. Nonetheless, the best way to manage OxyContin withdrawal symptoms is to seek medical help.
Tapering off opioids can help prevent severe withdrawal symptoms and shorten the OxyContin withdrawal timeline. Work with your doctor to create a tapering schedule based on your opioid use and health condition to wean off OxyContin safely and successfully.
That said, you should never attempt to stop taking OxyContin without medical supervision, as it may lead to life-threatening complications, such as severe dehydration.
Moreover, people dependent on opioids are at a very high risk of relapse, and going through the OxyContin withdrawal process on your own significantly increases this risk. This, coupled with the fact that relapse can lead to a potentially lethal overdose, means that it is crucial to seek professional help to safely detox from OxyContin and overcome opioid addiction.
Risks and Dangers of Taking OxyContin

Opioid abuse and addiction are among the greatest risks of taking OxyContin, which is why this medication is strictly regulated and classified as a Schedule II controlled substance.
According to the 2021 National Survey on Drug Use and Health (NSDUH) data, 2.6 million Americans (30.4% of all painkiller misusers) misused oxycodone products in 2021. It’s important to note that opioid abuse is both a precursor and a sign of opioid addiction.
Moreover, taking OxyContin can lead to an opioid overdose, a life-threatening emergency that kills 136 Americans daily. Given that oxycodone is a potent opioid, you may overdose on it by accidentally taking an extra dose. Also, if you relapse after detoxing from OxyContin, your typical dose may cause you to overdose due to decreased opioid tolerance.
Like any medication, OxyContin can also cause various side effects, including:
- Appetite loss
- Breathing problems
- Constipation
- Dizziness
- Drowsiness
- Fatigue
- Nausea
- Skin rashes
- Stomach ache
- Vomiting
To minimize the risk of OxyContin addiction, abuse, overdose, and side effects, always follow your doctor’s instructions when taking the medication.
Never mix oxycodone with alcohol or other substances, including vitamins and herbal medicines, without consulting with your doctor.
How to Detox From OxyContin
There are several ways you can detox from OxyContin, including medical detox, outpatient detox, and rapid detox.
Here’s how they differ:
- Medical detox. This type of detox typically involves round-the-clock medical supervision and, if needed, medications that help manage OxyContin withdrawal symptoms.
- Outpatient detox. In an outpatient detox program, you’ll essentially be given instructions on how to detox from OxyContin at home. You’ll likely need to visit the detox center at least once a week.
- Rapid detox. Rapid detox from OxyContin is an anesthesia-assisted medical procedure that flushes out opioids from the body in a matter of days.
However, OxyContin detox isn’t a cure for oxycodone addiction, and it often leads to relapse. Rather than treating opioid addiction, it simply clears out the substance from your system.
Meanwhile, Accelerated Neuro-Regulation (ANR) is an advanced opioid addiction treatment designed to bring your endorphin-receptor system back to balance. By addressing the root cause of opioid dependence, it negates the risk of relapse and ongoing withdrawal symptoms.
OxyContin Rapid Detox vs. ANR Treatment
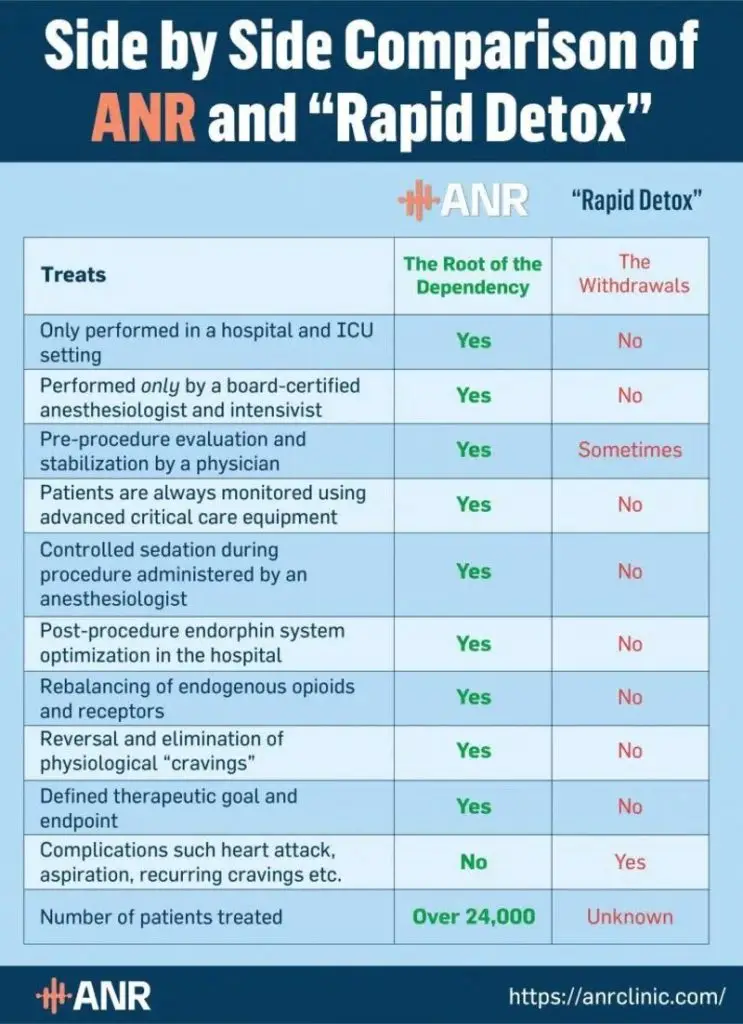
The key difference between OxyContin rapid detox and the ANR treatment is that, unlike rapid detox, ANR addresses the neurobiological root cause of addiction. By reversing the changes resulting in the brain from oxycodone use, it eliminates both withdrawal symptoms and the risk of relapse.
Meanwhile, the risk of relapse remains high after OxyContin rapid detox because this treatment doesn’t repair the imbalance in the endorphin-receptor system. This means that despite its high cost, rapid detox isn’t effective in helping you get off opioids for good.
Not to mention, the ANR treatment is much safer than OxyContin rapid detox, as it is always performed by board-certified medical professionals in an ICU setting in accredited hospitals. It is also tailored to your unique medical history and needs, making it safe even for those with complex health issues.
Here are more differences between OxyContin rapid detox and the ANR treatment:
ANR Opioid Treatment for OxyContin Addiction
Accelerated Neuro-Regulation (ANR) is a modern opioid dependency treatment that reverses the effects of OxyContin and restores your brain to its natural state.
Unlike detox treatments, such as rapid detox, the ANR method targets the mechanism behind dependency, attacking the issue at its core. This means patients can return to a normal, healthy daily life without chronic pain or fear of relapse.
ANR is the only form of medical treatment shown to re-regulate the critical endorphin-receptor imbalance found in those with opioid use disorder.
With an average hospital stay of 36 hours, ANR is much faster than long-term recovery treatments. Moreover, it negates the risk of overdose that can result from medically-assisted treatments like methadone replacement therapy.
ANR Clinic has healthcare facilities to provide our treatment in:
- DeSoto Memorial Hospital, Arcadia, Florida
- ANR Europe Thun, Switzerland
- New Vision University Hospital, Tbilisi, Georgia
- Goiania, Brazil
Starting your recovery journey with ANR is easy – all you have to do is contact us for a free consultation!
Key Takeaways
Ultimately, OxyContin detox is only the first step toward overcoming an opioid addiction. For a lasting recovery, it’s essential to restore normal brain function in addition to flushing opioids out of your system.
Currently, ANR is the only opioid addiction treatment that can help you achieve this—and it only takes a couple of days.
Here’s a summary of the key points we discussed:
- OxyContin is a brand name for the extended-release version of oxycodone, which is a potent opioid used for pain treatment.
- Nausea, runny nose, anxiety, cravings, depression, and body aches are some of the most common OxyContin withdrawal symptoms.
- OxyContin withdrawal symptoms tend to last longer than those of other opioids because of its extended-release formulation.
Additional Information:
OxyContin vs. Percocet: Key Differences & Similarities

