It’s not unusual for buprenorphine users to feel a false sense of security because of the widespread belief that it is less potent and addictive than other opioids. Still, it is an opioid, which means using it doesn’t come without risk, and buprenorphine addiction is one of these risks.
If you’re taking buprenorphine—be it for pain relief or as part of an opioid addiction treatment plan—it’s in your best interest to familiarize yourself with the risks associated with this medication.
This article will explain the key things you should know about buprenorphine dependence and addiction, from its signs and causes to prevention and treatment options.
What Is Buprenorphine?
Buprenorphine is an opioid drug prescribed to treat opioid use disorder (OUD) or pain that’s resistant to weaker, non-opioid painkillers. It is most commonly used in medication-assisted treatment (MAT), where patients addicted to opioids attend behavioral therapy and counseling in addition to taking the medication.
Like hydrocodone and oxycodone, buprenorphine is a semi-synthetic drug derived from thebaine, an alkaloid found in poppy plants.
However, unlike most opioids, buprenorphine is a partial opioid agonist, meaning it doesn’t activate opioid receptors to the same extent as full opioid agonists. Thanks to this, it is less likely to induce the intense euphoria associated with opioids.
Due to its properties, the effects of buprenorphine plateau at higher doses. This “ceiling effect” reduces the risk of buprenorphine abuse, which is why it is generally regarded as a safer alternative to methadone.
Buprenorphine is available in several forms, including:
- Sublingual tablets (Subutex®)
- Skin patches (Butrans®)
- Subdermal implants (Probuphine®)
Some buprenorphine products like Suboxone® also include naloxone, a drug that blocks the effects of opioids, reversing an opioid overdose.
When used as intended, buprenorphine and its products can reduce withdrawal symptoms, including cravings, helping people quit more potent opioids. It can also lessen the risk of opioid abuse and overdose.
Side Effects of Using Buprenorphine
Whether you’re taking buprenorphine for pain relief or opioid addiction treatment, you may experience various side effects, such as:
- Stomach ache
- Constipation
- Nausea
- Vomiting
- Drowsiness
- Excessive sweating
- Sleep disturbances
- Headache
- Lightheadedness
- Confusion
Inform your doctor about any unwanted effects you experience while taking buprenorphine. In case of an allergic reaction, difficulty breathing, or other severe side effects, seek medical attention immediately.
Furthermore, long-term use of buprenorphine may put you at a higher risk of:
- Buprenorphine abuse, dependence, and addiction
- Breathing problems
- Organ damage (e.g., liver or kidney failure)
- Opioid overdose
- Coma
- Death
Is Buprenorphine Addictive?
Buprenorphine is addictive, even though it is used to treat opioid addiction. While taking it as prescribed reduces the risk of overdose and death, it’s not unheard of for patients in buprenorphine rehab to end up swapping one addiction to opioids for another.
Due to its potential for addiction, buprenorphine is treated as a Schedule III controlled substance in the United States.
While it is less likely to lead to abuse and overdose than most opioids, it can still be misused, which increases the risk of buprenorphine dependence. People often abuse it by crushing buprenorphine tablets and injecting or snorting them instead of taking them sublingually.
Meanwhile, Suboxone® abuse is less common, as abusing this drug causes naloxone to be released into the system. Rather than making users feel “high,” this triggers uncomfortable opioid withdrawal symptoms.
The bottom line is that buprenorphine is an opioid, even though it produces weaker effects than full opioid agonists like morphine, fentanyl, etc. As such, it can still lead to addiction, especially when misused.
Buprenorphine Abuse Statistics
Let’s take a look at some statistics that reveal the extent of buprenorphine use, abuse, and accessibility in the United States:
- In 2022, roughly 20% of Americans using buprenorphine products for any reason abused their medication.
- Between July 2019 and July 2021, 1955 drug overdose deaths involved buprenorphine, with nearly 93% of them also involving other substances.
- In 2019, less than 18% of Americans addicted to opioids received medications such as buprenorphine.
- Between 2003 and 2015, the percentage of opioid treatment programs (OTPs) offering buprenorphine increased by 47%.
Buprenorphine Addiction Signs and Symptoms
Buprenorphine addiction can manifest in various symptoms, some of which can be easier to recognize than others.
If you or someone you love is taking buprenorphine, here are some physical and behavioral signs and symptoms you shouldn’t ignore:
Buprenorphine Addiction Physical Symptoms
As with any type of opioid dependence, people addicted to buprenorphine will experience withdrawal symptoms once they stop taking their medication.
If you experience cravings, flu-like symptoms, agitation, and other physical and psychological symptoms after discontinuing medication use, you should seek professional help to minimize the risk of relapse.
Other physical symptoms of buprenorphine abuse and addiction may include:
- Unexplained, sudden weight loss
- Slurred speech
- Problems with coordination
- Itching
- Constipation
- Drowsiness
- Changes in appetite
- Breathing problems
- Dilated pupils
People addicted to buprenorphine will also often experience psychological symptoms such as depression, anxiety, rapid mood swings, and the exacerbation of mental health issues.
Buprenorphine Addiction Behavioral Symptoms
The following behaviors may indicate that you or a loved one is struggling with an addiction to buprenorphine:
- Going to different doctors to obtain a prescription for buprenorphine
- Lying about the extent of buprenorphine use or hiding it from others
- Becoming isolated from loved ones
- Neglecting professional and personal responsibilities
- Losing interest in hobbies and other previously enjoyed activities
- Having trouble cutting back on or stopping buprenorphine use
- Being preoccupied with obtaining and using buprenorphine
- Using more buprenorphine than prescribed or taking it more frequently than directed
Buprenorphine Addiction vs. Buprenorphine Dependence
Even though the terms “buprenorphine addiction” and “buprenorphine dependence” are often used interchangeably, there’s a difference between the two.
Specifically, buprenorphine dependence is physical in nature and signifies that the body can’t function normally without the drug. It is characterized by two main symptoms: tolerance and withdrawal symptoms, which appear when people dependent on buprenorphine stop taking it.
Buprenorphine addiction, meanwhile, manifests in both physical and psychological symptoms. Over time, buprenorphine dependence may develop into an addiction, so it’s in your best interest to seek professional help if you suspect you may be dependent on this medication.
Buprenorphine Addiction Causes and Risk Factors
The root cause of buprenorphine dependence and addiction is the imbalance that results in the brain due to buprenorphine use, which means anyone taking it risks becoming addicted.
Every opioid has the potential to cause addiction because they all affect the brain in the same way. Buprenorphine is no exception.
Our body produces endorphins as a response to various stimuli: pain, pleasure, stress, excitement, etc. Endorphins reduce pain and cause a feeling of relaxation. Opioids have the same effect—they affect endorphin receptors, causing the body to adapt over time and stop producing natural endorphins.
As more opioids are introduced into the body, more opioid receptors are created. This leads to tolerance and creates a self-perpetuating cycle of demand and supply, as your body requires larger doses of the drug to feel its effects.
Tolerance is a sign of buprenorphine dependence, which can eventually turn into an addiction.
You may also be at a higher risk of becoming addicted to this medication if you:
- Have a family history of substance abuse
- Can easily access buprenorphine
- Have been exposed to opioids or other substances from a young age
Buprenorphine Withdrawal Symptoms
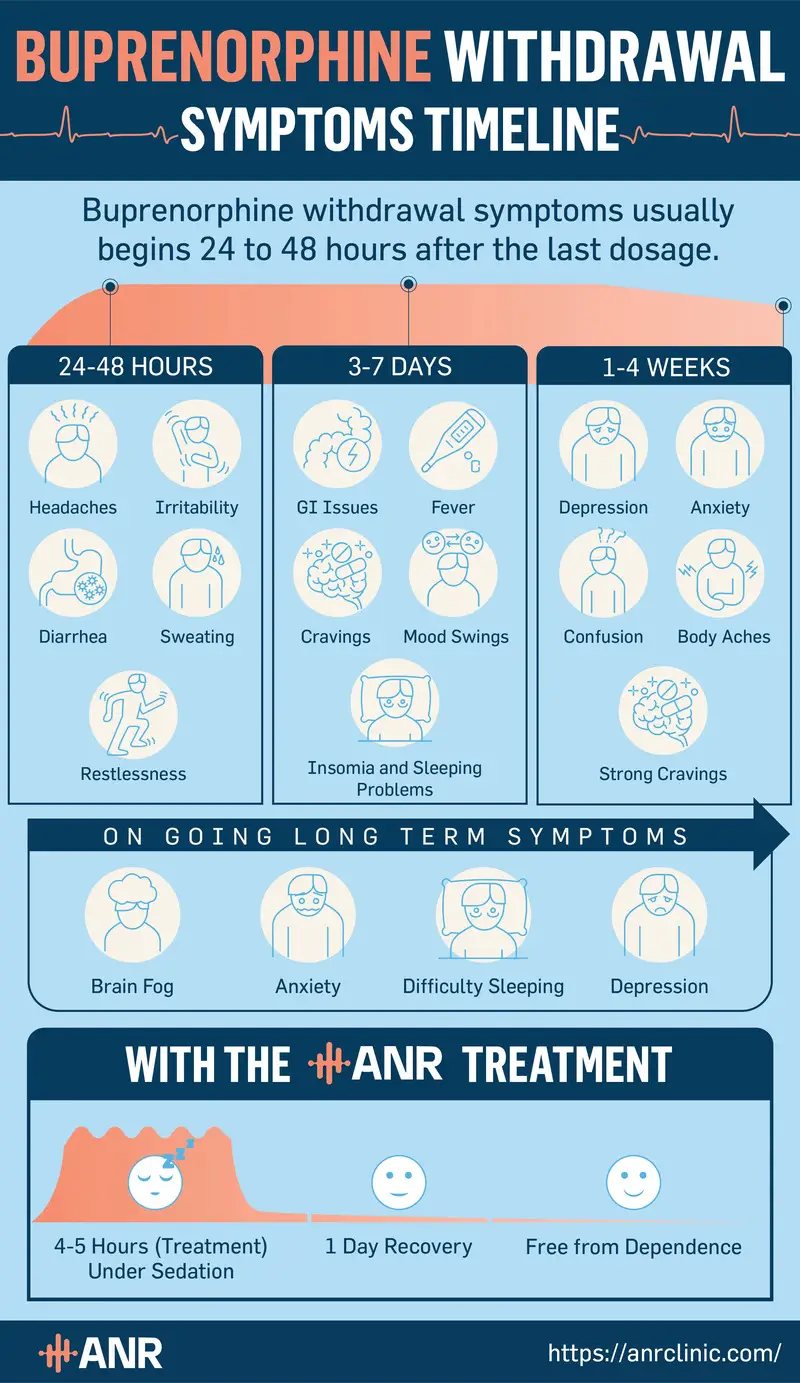
Even though buprenorphine is often used to reduce opioid withdrawal symptoms, it can also cause them—especially if you stop taking your medication suddenly after becoming addicted to it.
Not only that, but buprenorphine can also induce precipitated withdrawal symptoms if administered too early. For this reason, it’s important to ensure that patients are already experiencing mild-to-moderate withdrawal before initiating buprenorphine therapy.
Since it is a long-acting opioid, buprenorphine withdrawal symptoms usually start within the first two days after taking the last dose and normally last around a month.
Buprenorphine can induce both physical and psychological withdrawal symptoms, with the most common ones being:
- Cravings
- Flu-like symptoms like runny nose
- Depression and anxiety
- Body aches
- Diarrhea
- Fever
- Nausea
- Vomiting
- Dilated pupils
- Yawning
- Sweating
- Trouble falling and staying asleep
Buprenorphine withdrawal symptoms can be tough to manage on your own, and doing so can put you at an increased risk of relapse, overdose, and even death. Because of these risks, you should never attempt to quit your medication without medical supervision.
Risks of Buprenorphine Overdose
The fact that buprenorphine produces milder effects than full opioid agonists like oxycodone doesn’t rule out the possibility of an opioid overdose.
While it is relatively rare, a buprenorphine overdose can happen if you take a larger dose of the drug than your body can safely metabolize. Usually, this happens due to buprenorphine abuse.
Most buprenorphine overdose deaths involve other substances besides it, which is why you should never mix your medication with alcohol, benzodiazepines, or other drugs.
Also, you should never take buprenorphine without a prescription, especially if you have a low tolerance to opioids, as this could cause you to overdose.
People overdosing on buprenorphine may display the following signs:
- Cold, clammy skin
- Pale, discolored lips and fingernails
- Low blood pressure
- Constricted pupils
- Extreme drowsiness
- Difficulty breathing
- Seizures
- Loss of consciousness
- Vomiting
- Severe confusion
A buprenorphine overdose can be lethal if not reversed promptly. If you suspect you or someone else may be overdosing, call 911 immediately.
How to Prevent Buprenorphine Addiction
If you’re taking buprenorphine, here’s what you can do to reduce the risk of buprenorphine dependence and addiction:
- Take buprenorphine responsibly. Carefully follow your doctor’s instructions when taking your medication, and track your intake to make sure you don’t take an extra dose by accident. Do not mix buprenorphine with other substances or increase your dosage without your doctor’s approval.
- Keep in touch with your doctor. Inform your doctor about any side effects you experience after taking buprenorphine, especially if they are severe or don’t resolve quickly. Talk to your doctor if you need to take other types of medications, herbal medicines, or supplements to ensure they can be taken with buprenorphine.
- Handle your medication correctly. Always make sure you store buprenorphine out of the reach of pets and children. Also, if you have any unused or expired medications, dispose of them safely.
That said, the only guaranteed way to ensure you don’t get addicted to buprenorphine is not to take this medication in the first place.
If you’re suffering from pain, see if there are any non-opioid alternatives for pain management your doctor could recommend.
If you’re struggling with an addiction to opioids and are considering taking buprenorphine, consider exploring opioid dependence treatments that do not involve opioid replacement drugs, such as Accelerated Neuro-Regulation (ANR).
ANR Treatment for Buprenorphine Dependence
Are you looking for a safe and effective buprenorphine dependence treatment that can help you overcome opioid dependence quickly?
Consider undergoing Accelerated Neuro-Regulation (ANR), an innovative treatment for opioid dependence that tackles its root cause.
The ANR treatment re-regulates the endorphin-receptor system to its normal levels, bringing the brain to its pre-dependence state. As a result, it eliminates withdrawal symptoms, allowing you to leave the fear of relapse in the past.
Carried out in an ICU setting of accredited hospitals, ANR is performed under sedation by highly experienced medical professionals. Our patients are hospitalized for only 36 hours on average, meaning ANR can help you overcome opioid dependence in a matter of days!
Moreover, each ANR treatment is personalized according to the patient’s needs and medical history, negating the risk of side effects. This, coupled with the fact that our team consists of cardiologists, nephrologists, and other healthcare experts, means that it can be safely performed even on those with complex health issues.
For more information, contact us today and book a free consultation!
Key Takeaways
If you have to take buprenorphine, remember to do so responsibly and follow your doctor’s recommendations to minimize the risk of buprenorphine dependence and addiction.
Lastly, let’s briefly wrap up what we covered today:
- Buprenorphine is a semi-synthetic opioid prescribed either for pain relief or opioid addiction treatment, usually in MAT.
- Buprenorphine alters the brain in the same way as other opioids, which is why it can be potentially addictive.
- The ANR treatment can help you overcome an addiction to any type of opioid, including buprenorphine, without exposing you to the risk of getting addicted to opioid replacement drugs.
Buprenorphine Addiction FAQ
1. Can you abuse buprenorphine?
Buprenorphine can be abused, even though it carries a lower potential for abuse and addiction than most other opioids. Most commonly, people abuse it by snorting or injecting crushed tablets and combining it with alcohol or other substances. Buprenorphine abuse dramatically increases the risk of addiction and overdose.
2. Why is buprenorphine a narcotic?
Buprenorphine is a narcotic because it belongs to the family of opioids and has analgesic properties. However, the CDC recommends using the term “opioids” instead to avoid confusion with illegal drugs.
3. What is the 3-day rule for buprenorphine?
The three-day rule for buprenorphine (21 CFR 1306.07(b)) regulates how and when physicians can dispense this medication for emergency treatment. The rule allows physicians to dispense no more than three days' worth of buprenorphine to patients waiting to initiate maintenance or detoxification treatment.
4. Is it okay to store buprenorphine for a long time?
You should only store buprenorphine for as long as it is part of your treatment plan for pain or addiction to opioids. If you no longer need to use buprenorphine or it has expired, you should stop taking it and discard any excess you have.
5. Does buprenorphine help with sleep?
Buprenorphine can help with sleep, especially if pain keeps you awake. However, it is not a sleep aid and should not be used as such. While people taking it may experience feelings of relaxation and drowsiness, it can also cause insomnia once discontinued.
6. What is the correct dosage for buprenorphine?
Your doctor can help you determine the correct dosage for buprenorphine. After assessing your physical and psychological symptoms, they will prescribe you the correct dose if you need it.
7. Are methadone and buprenorphine the same medicine?
Methadone and buprenorphine aren’t the same medicine, even though they are both used to replace other opioids in medication-assisted treatment. Methadone is a fully synthetic drug, whereas buprenorphine is synthesized from thebaine. Recently, methadone has been used less and less due to its high abuse and overdose potential.
8. What are naloxone/buprenorphine combination products?
Naloxone/buprenorphine combination products like Suboxone® and Zubsolv® are FDA-approved medications used to treat opioid addiction. They were developed to mitigate the potential for misuse associated with buprenorphine-only products. Because they contain naloxone, abusing these medications causes the user to experience withdrawal symptoms.
9. Are Suboxone® and Subutex® the same?
Suboxone® and Subutex® are not the same, although both of these drugs contain buprenorphine. However, Suboxone® also contains naloxone. Due to its lower potential for abuse, it has become a more widely used and favored medicine among doctors across the United States.
10. Can you overdose on Suboxone®?
Yes, you can overdose on Suboxone®, just as you can overdose on other buprenorphine brands or street drugs containing buprenorphine. While it isn’t common, abusing the drug, mixing it with other substances, and taking it if you have a low tolerance to opioids increases the risk of a Suboxone® overdose.
11. Can prescription opioids cause neonatal abstinence syndrome?
Yes, prescription opioids can cause neonatal abstinence syndrome (NAS). This syndrome occurs when a baby experiences withdrawals from substances it was exposed to in the womb. This is often found in babies whose mothers abused opioids during pregnancy.
